Cartilage damage can be very painful, but paradoxically it doesn’t have to be. The reason: the cartilage layer itself is completely insensitive to pain. Cartilage defects are therefore often only perceived as painful when the cartilage layer has already been worn away and destroyed and bones are rubbing against each other without protection.
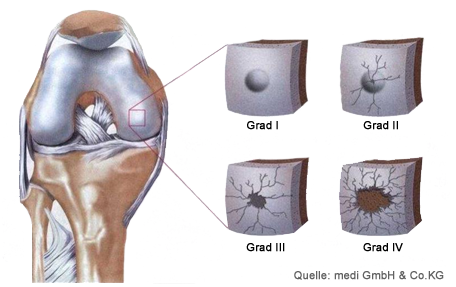
The location of the cartilage damage is decisive for the symptoms of cartilage damage. If it is located in areas subject to heavy strain, symptoms are more likely to occur than if the damage is in areas subject to less strain. Another important factor influencing the symptoms of cartilage damage is the extent or size of the cartilage defect.
The key factor in cartilage damage is that the cartilage’s ability to regenerate is very limited. Once the cartilage is damaged, it hardly regenerates on its own. Injured or destroyed cartilage does not grow back in its original form. To make matters worse, damaged cartilage – if left untreated – usually spreads further. However, if diagnosed and treated in good time, cartilage damage can be successfully halted in many cases and consequential damage avoided.